When you’re in a relationship with someone, it’s important to have at least some idea of how you want to go ahead with it.
There can be confusion and butting of heads, and you ought to make sure that you don’t let dealbreakers go unnoticed and unaddressed, such as whether you want to have kids or not. If not, is a vasectomy an answer, and is it even safe?
The failure rate for a vasectomy is extremely low, though whether it does fail may be influenced by various factors.
These factors may be the result of having sex too soon, or simply due to a medical error in the surgical process.
Table of Contents
How often does a vasectomy fail?
Vasectomies are a highly effective means by which to prevent pregnancy, with a success rate of approximately 99.85 percent.
Of course, anything less than a 100 percent success rate is, of course, going to have at least some risk.
The overall process of a vasectomy involves snipping the vas deferens – the tube that allows your mature sperm to reach your urethra – and tying off both ends, thereby (in nearly all cases) preventing it from making the journey.
Is there any way to lower the risk of a vasectomy failing?

There are some freak incidents where the vas deferens reforms on its own, or a doctor failed to do the surgery properly, but regardless of how likely the vasectomy is to succeed, you are still strongly advised to follow some precautions.
During the first two months, you need to make sure that you avoid having sex with someone who can get pregnant.
If you can’t help it, at least make sure that you use a condom or a diaphragm, to reduce the likelihood of a functional vas deferens giving you a surprise impregnation.
After those two couple months, your doctor will take a look at your semen, attempting to see if there is any sperm present in it.
Following this initial check, you will need to be checked again either at the three-month mark or 20 ejaculations (whichever comes first).
The reason why you need to be cautious about the point immediately following your surgery is that there may still be sperm in your vas deferens for weeks or months, so before you can safely have unprotected sex, you need to make sure that it is completely clear of it.
What happens if my vasectomy does not work the first time around?
In the event that your vas deferens reforms or the process was incorrectly done leading to it not being properly snipped and tied, you may have to undergo a second surgery to rectify the issue(s).
This is an extremely unlikely scenario, so don’t worry too much about whether you or your partner will end up needing it redone.
Are vasectomies safe?

Vasectomies are not particularly unsafe, only as unsafe as any surgery you may experience. And like any surgery, there are some risks you should consider.
For instance, you may suffer an infection, though such a thing is easily treated with antibiotics.
There are other risks that may rear their heads resulting from the surgery, such as bleeding, swelling, pressure in your testes, pain, bruising, and more.
With pain, a small percentage of people who get a vasectomy experience a syndrome called post-vasectomy pain syndrome, wherein the patient experiences persistent pain following the procedure, in some cases even if the procedure is reversed.
Vasectomies can be made less safe if done in an improper way.
For example, if you have a scrotal infection, wait until the infection clears up before undergoing this procedure.
Regardless of how you feel about the surgery, any surgery should only be undertaken once you have given informed consent and are made aware of the potential risks and benefits of doing so.
How safe are vasectomies compared to tubal ligation?
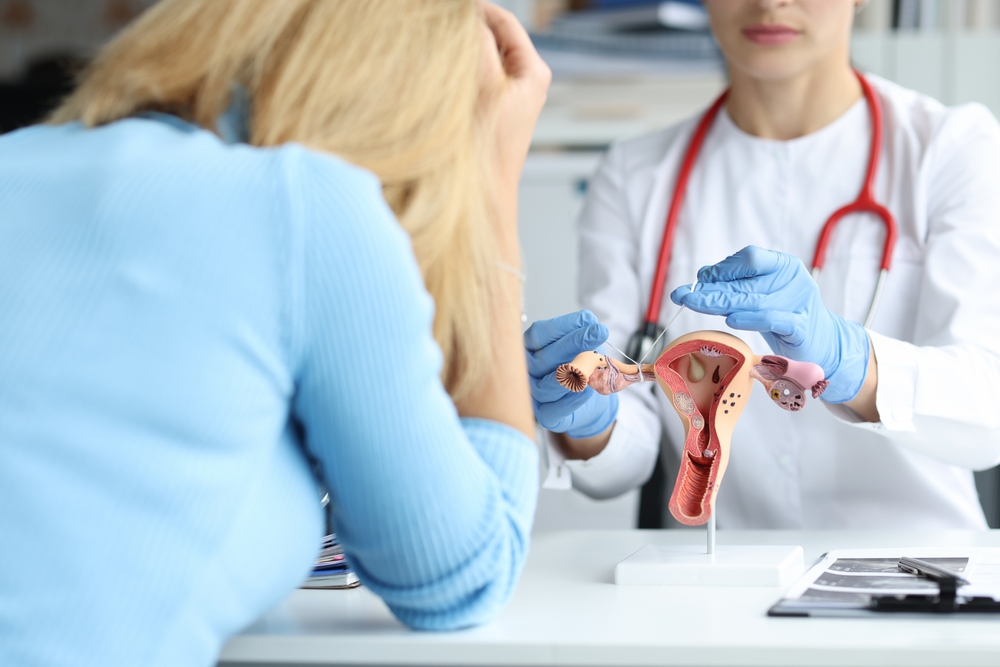
Where men typically undergo vasectomies in order to prevent them from having children, the typical surgical alternative for women is to look into getting a tubal ligation (more commonly known as getting one’s tubes tied).
The process involves tying the fallopian tubes, which means that the eggs are not able to travel to the uterus in preparation to be fertilized.
In the grand scheme of things, vasectomies and tubal ligation are both risky, but tubal ligation is more so.
This is because tubal ligation is a more invasive process, thereby introducing a greater collection of potential complications that may arise.
Tubal ligation is also a longer process than a vasectomy and requires the use of anesthesia.
Tubal ligation, while comparably effective in terms of preventing pregnancy, may have a wider range of potential pregnancies than a vasectomy has.
Thus, going this route may mean that you could be more likely to have an unintended pregnancy.
Still, it is not a massive difference, so that should not be a massive factor in the decision process between the two procedures.
Can vasectomies be reversed?
In nearly all cases, vasectomies can be reversed; however, you need to enter into this procedure knowing that you may not be able to conceive afterward.
Not only is that an issue, but the longer you wait to get the procedure reversed, the less likely you are to be able to conceive.
The likelihood of pregnancy after a vasectomy varies from as low as 30 percent to as high as 90 percent.
Of course, you also need to factor in the age of your partner, as well as the skill level of the person performing the reversal process.
If you had fertility issues even before you got the vasectomy, this will likely play a role in these fertility struggles.
The process of reversing the vasectomy is only about as risky as it is to get the vasectomy done in the first place – pain, bleeding, and infection are all something you should be aware of as potential risks.
It may also be a more complicated procedure than you had undergone the first time around called a vasoepididymostomy, wherein the van deferens is reattached to the testicles.
Overall, your insurance provider may deem that this is not under their purview and decline to cover the procedure.
Is there a form of male birth control?

Over time, progress has been made with respect to birth control for men that would decrease the risk of pregnancy even further than it is with the protection we have now.
There are a lot of issues that have come up with developing male birth control.
First, doing it through injection is an unappealing method, and thus would be unlikely to get a lot of use by men.
Even with pill-based male birth control, there are a lot of side effects that need to be considered, such as how they affect the liver, which keeps them from being approved for use.
Progress towards male birth control that has no side effects and are convenient is promising, and hopefully, safe progress can be made soon.




